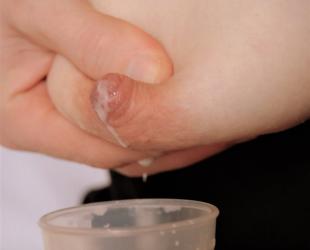
Expressing colostrum before birth may help your baby in the early days after birth.

It’s possible to express your colostrum before your baby arrives. This is called antenatal expressing. It means you collect and freeze your colostrum while you’re still pregnant, so it’s ready if your newborn needs it.
Colostrum is the first milk your breasts make, from around the 16th week of pregnancy. It’s packed with immune factors and helps your baby’s gut develop healthy bacteria, which can protect against allergies and illness.
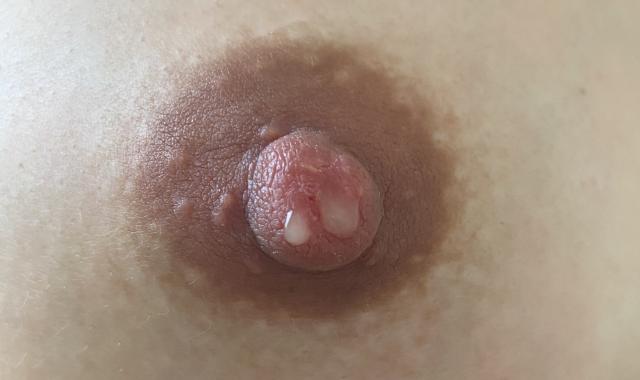
Why might you express colostrum before birth?
Most mums can breastfeed soon after birth. But sometimes, babies need extra fluids in the early days. Having your own colostrum ready means you can avoid using formula if your baby needs more than they can get directly from you.
Your midwife or obstetrician might suggest expressing colostrum before birth if:
- You have diabetes during pregnancy. Babies born to mums with diabetes can have low blood sugar after birth. Extra colostrum can help keep their blood sugar stable.
- Your baby has a condition that might make feeding more difficult. This could include a cleft lip or palate, or certain heart or neurological conditions. If your baby is diagnosed with one of these before birth, having colostrum on hand can be helpful.
Always talk to your midwife or obstetrician before you start expressing colostrum in pregnancy.
Is antenatal expressing safe?
A large Australian study (the DAME study) found that women with diabetes and a low-risk pregnancy can safely express colostrum in late pregnancy. It didn’t cause harm to their babies. Some first-time mums who expressed colostrum were also less likely to need formula in the first 24 hours after birth.
Check with your healthcare provider to make sure antenatal expressing is a safe option for you.
When and how to express colostrum
Most mums are advised to wait until late in pregnancy before starting. Colostrum is thick and comes in small amounts, so hand expressing usually works best. You can collect it onto a spoon, into a small cup, or use a syringe to draw up drops straight from the nipple.
The amounts of colostrum you collect will be very small. If you aren't able to collect much, it doesn't mean you'll have any problems with breastfeeding later.
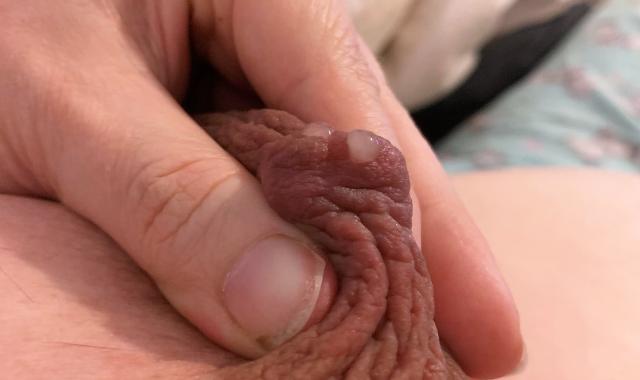
Learn how to hand express colostrum.
The information on this website does not replace advice from your health care provider.
© Australian Breastfeeding Association February 2026
Forster DA, Moorhead AM, Jacobs SE, Davis PG, Walker SP, McEgan KM, Opie GF, Donath SM, Gold L, McNamara C, Aylward A, Ford R, Amir LH 2017, Advising women with diabetes in pregnancy to express breastmilk in late pregnancy (Diabetes and Antenatal Milk Expressing [DAME]): a multicentre, unblinded, randomised controlled trial. The Lancet, 389(10085): 2204-2213. https://doi.org/10.1016/S0140-6736(17)31373-9
Learn more to prepare for breastfeeding