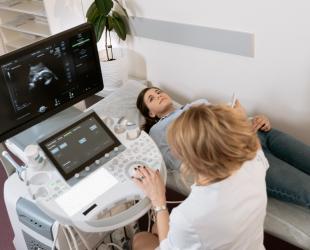
If someone in your family needs hospital care, you may need breastfeeding support
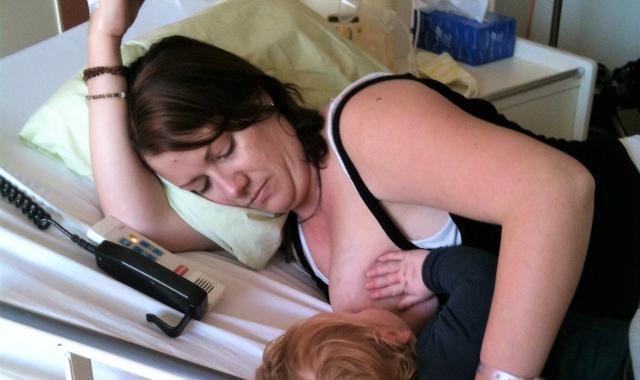
If you or your child needs hospital care, it’s natural for you to worry it will affect breastfeeding.
On top of the health concerns, you may also have questions about breastfeeding, expressing milk and sometimes even weaning. The unknown parts often cause the most worry, so it’s helpful to plan ahead.
Let hospital staff know you are breastfeeding
Whether it is you, your baby or your older child who needs to go to hospital, tell your doctor that you are breastfeeding. Ask that you and your baby be kept together wherever possible. Hospitals usually have policies which allow mothers to keep breastfeeding. However, staff may need special permission if normal procedures need to be changed.
Unless your medical condition is urgent, use the time beforehand to make a plan with hospital staff that doesn't disrupt breastfeeding too much.
Make sure nursing staff know you are breastfeeding.
This should be written on the treatment form, for when staff change. If you need to, add it yourself when you sign the form.
Also let the doctor, surgeon and anesthetist know. This will help them to plan your care and choose medicines for you that are safe for breastfeeding.
Hospital accommodation
Public hospital policies usually allow mothers and breastfed babies to stay together. However, where COVID-19 restrictions apply, policies may have changed. Check with your hospital what they allow.
The accommodation and facilities available depend on the individual hospital or ward. There may be rooms set aside or just a folding bed or a reclining chair, either in the ward or nearby. Ask if meals are provided or can be bought cheaply from a canteen or from the staff dining room. Is there family accommodation nearby?
The cost of private hospitals will vary. It is wise to find out early how much you will need to pay. Check what costs are covered by your health fund, especially if you will need to have a private room to keep your baby with you.
Unless it is your baby who is the patient, you will probably need to supply everything your baby needs, including a pram or portable cot for sleeping. Take your breast pump, if you have one, along with milk containers, wipes and a hand towel.
If you live in a rural area, you may have some travel and accommodation costs reimbursed by government schemes to assist isolated families. Ask your local health or human services departments or a social worker at your hospital about the assistance available in your state or territory.
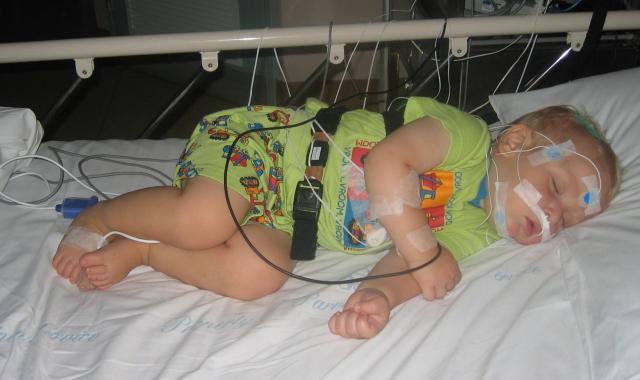
When your breastfed baby or toddler is hospitalised
Doctors and hospitals now accept that a baby or child in hospital needs to have their mother close, especially when they are breastfed.
- Your breast is a familiar and secure place.
- Breastfeeding will help your baby cope better with any pain or discomfort from hospital procedures.
- Breastfeeding provides excellent nutrition and hydration and is easy for a sick baby to digest.
- Antibodies and other factors in your breastmilk will help your baby’s recovery. If they need surgery, breastfeeding lessens the risk of complications and helps them to heal and recover more quickly.

Preparing for baby’s surgery
A baby normally needs to fast for several hours before having anaesthesia for surgery. Discuss with your anaesthetist when breastfeeding will be allowed.
It is easier if surgery is done as early as possible in the morning, preferably after your baby fasts at home. Wherever you are, it may be easier if someone else cares for your baby while you stay out of sight. Fasting can be stressful if your baby is used to sleeping with you, waking and feeding frequently during the night.
After baby's surgery
Check if you can be with your baby in recovery and how soon they can breastfeed. Toddlers coming out of an anaesthetic are often disorientated and upset. A breastfeed can be calming and soothing.
Some babies don’t want to feed for a while after surgery. Tell the hospital staff if this happens so they can make sure that baby has enough fluids. Express to keep your breasts comfortable and keep up your supply until they are ready to breastfeed again. Ask the nursing staff for somewhere private to express if you’d prefer.
If your child has a drip or their treatment makes it difficult for them to move, you may have to try different feeding positions. Ask the nursing staff to help you position baby so that you can breastfeed without disturbing bandages or equipment. Breastfeeding can be a good way to keep older babies or toddlers calm and still and may reduce any need for sedatives.
If your baby is in isolation, ask the nursing staff to show you the procedures you need to follow so that you can be with them.
If you need to leave baby
If you cannot stay with your baby all the time, you will need to leave some expressed breastmilk (EBM) for staff to feed them when you are not there. If your baby hasn’t had milk from a bottle before, you may like to ask for them to be fed your expressed breastmilk (EBM) by cup. This helps avoid possible problems when you return to breastfeeding that are sometimes caused by the faster flow rate and different type of sucking needed for the bottle.
When your older child is hospitalised
What do you do if you want to stay with your sick child and you have a breastfed baby? This depends on the needs of your hospitalised child and the amount of time you need to spend there. Each situation is different.
Very young babies can usually be carried in a sling or kept close to you in a pram. If there is room, older, more mobile babies may be happy in a portable cot for both sleep and play. If you can, take regular breaks. Go for a walk or have a relative or friend look after baby for part of the day or between feeds. Even if there is a play space in the ward, your sick child will probably want you close by.
When you are breastfeeding twins and one is hospitalised, your doctor might agree to have the other admitted as well, or arrange for you to keep both babies with you.
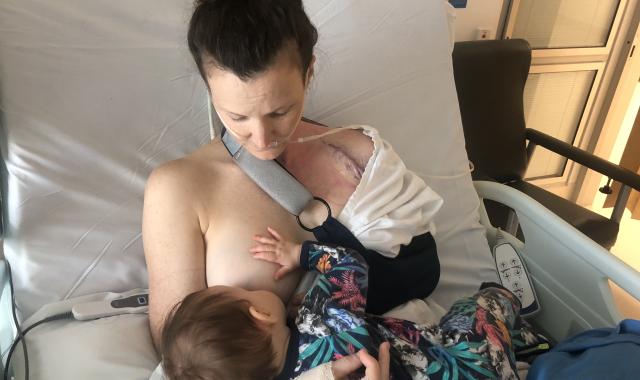
When you are hospitalised
If you have to go to hospital, you may have an extra worry — how will you be able to keep breastfeeding? In almost all cases it is possible to keep your supply up, and better if you do. Sudden weaning can be very distressing for both you and your baby. It puts you at risk of engorgement and mastitis, while some babies are so upset that they cry for long periods and may refuse bottles or other food.
Planning ahead
Going to hospital is often stressful and tiring. If you have time to plan ahead, express and freeze some breastmilk. This will be a useful backup if your supply drops for a while or if you cannot breastfeed for any reason.
Most mums find that even if their supply does drop while they are in hospital, it soon comes up again when they are back at home and feeding normally.
If you are having surgery
You may be able to choose when to go to hospital or have surgery. Sometimes it is easier when a baby is older and can be cared for by someone else away from the hospital, at least during the day. Many minor operations can be done as day surgery.
If you are having surgery, you are likely to need to fast (have no food or drink) for several hours beforehand. Discuss this with your anaesthetist so you can plan when to breastfeed. Check when you can return to breastfeeding after anaesthesia. Often it is safe to resume as soon as you are awake and alert.
If you are too sick to have your baby with you (or the hospital doesn’t allow it), ask staff or your partner to help you express your breasts often. Have your baby brought in for visits and breastfeeds as often as possible.
A short-term drop in milk supply is common after illness or surgery. Often the supply quickly returns to normal, either in hospital or soon after you get home. More frequent feeds and plenty of rest will rebuild your supply to meet your baby’s needs in a few days. In fact, even if you have had to wean temporarily, it is possible to start breastfeeding again.
Drugs
Most medicines only pass into breastmilk at low levels and won't affect the baby. It is rare that you would have to stop breastfeeding completely. Discuss all prescribed medicines with your doctors to make sure they are safe while breastfeeding. If your doctor is unsure, ask that they check with drug information experts.
Co-sleeping while taking medications that make you drowsy is unsafe and should be avoided.
Going home
It will take time to get back to normal after you go home. Your children may be unsettled and ‘clingy’ or they may be angry and have tantrums. They may need extra reassurance and more cuddles and breastfeeds than usual. You may feel very tired.
Follow your doctor’s advice about resting and allow yourself time to recover. The less you do, the faster you will get better. Ask others to help with lifting, cleaning and making meals. Breastfeeding gives you a wonderful opportunity to sit or lie down and relax while you are recovering.
© Australian Breastfeeding Association April 2024
Ghosh, B., Sripathi, S., Nuthalapati, B. S., Dwivedi, A., Pandey, A., & Sarkar, P. (2024). Effects of breastfeeding in postoperative complication in pediatric population: A systematic review. Annals of Medicine and Surgery (2012), 86(4), 2124–2129. https://doi.org/10.1097/MS9.0000000000001829
Bartick, M., Hernández-Aguilar, M. T., Wight, N., Mitchell, K. B., Simon, L., Hanley, L., Meltzer-Brody, S., & Lawrence, R. M. (2021). ABM Clinical Protocol #35: Supporting breastfeeding during maternal or child hospitalization. Breastfeeding Medicine, 16(9), 664–674. https://doi.org/10.1089/bfm.2021.29190.mba