The key to getting more milk is triggering your let-down reflex.
Relaxation, warmth and gentle massage can help.
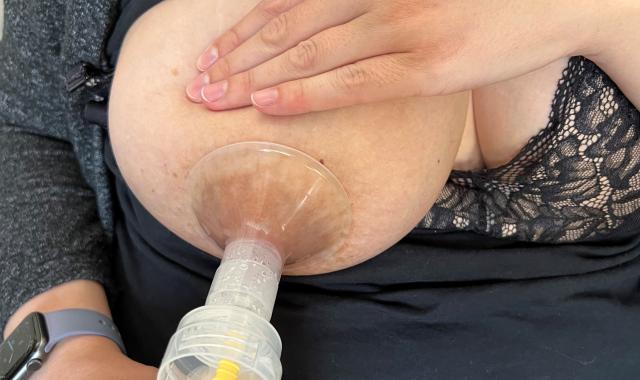
Many mums find they can only express a tiny amount. This doesn’t mean they don't have any milk. It's often because their let-down reflex hasn’t yet been triggered so the milk doesn’t flow.
Your let-down is a conditioned response. This is a good thing because there are so many steps you can take to encourage it!
Helping your milk to flow
Normally, your baby plays a big role in assisting your let-down. When you're expressing, you may need some help to get your milk to flow.
Try these suggestions.

Try to relax using whatever method suits you
If possible, pump in a quiet, warm, relaxing area, away from distractions. While expressing, breathe slowly and deeply.
You could express in the place you usually sit to feed. Some mums have a warm drink first or listen to soft music.
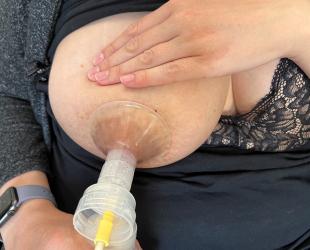
Use warmth and gentle massage
Express after a warm shower, pop a warm washer on the breast for a few minutes before starting.
Stroke down from your chest towards the nipple or draw your nipple out gently between your fingers. While you can't actually push the milk out of your breasts by massage, you can help trigger the let-down by touching your breasts and nipples.
Think about your baby
If you are away from your baby, looking at a photo or video of them can help. Having a blanket that has been in your baby’s cot may help, as the smell reminds you of your baby.
If baby is premature or sick in hospital, you might find it easier to pump near their cot or just after you leave them.
These are all triggers for the let-down reflex.

Distract yourself by watching or reading something
Talk on the phone, watch a video or do some other activity. This may stop you from worrying about how much milk you are expressing.
Some mums have more success if they cover the pump with a cloth, so they don't keep checking it and worrying about how much is coming out! The key for many women is being relaxed.

Have someone to support you
Many mums find they manage much better when they have an encouraging partner or friend.
Read more about expressing and storing
Evidence-led info and practical tips from our Breastfeeding Information Series
Breastfeeding: expressing and storing breastmilk

© Australian Breastfeeding Association April 2022

