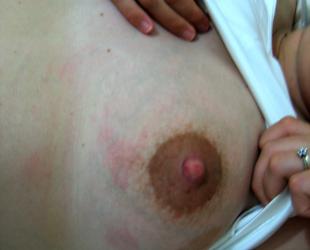
Feeling unwell with a sore, red breast or damaged nipples?

Mastitis is inflammation of the breast tissue. It is a step on from localised breast inflammation and may arise from engorgement, damaged nipples or overfull breasts. Sometimes a bacterial infection is present but not always.
Symptoms of mastitis
You will usually feel unwell with flu-like symptoms such as a fever, chills or fast heart rate.
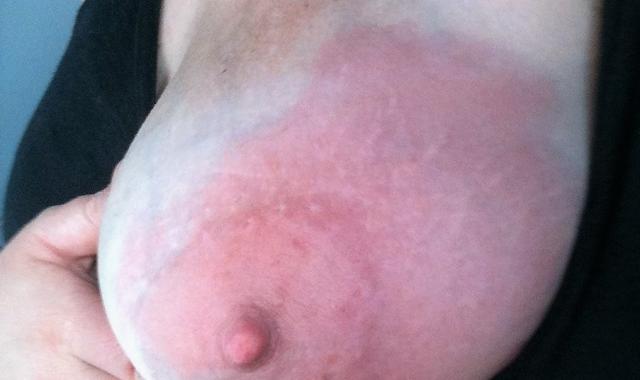
Part of your breast may look red and swollen. The skin may be shiny or have red streaks.
Your breast can feel hot and painful.
Mastitis can come on quickly—sometimes feeling unwell is the first sign, even if you haven’t noticed early breast inflammation.
If you don’t start to feel better (or get worse) within 12 to 24 hours, or if you feel very unwell, see a doctor. Untreated mastitis can lead to a breast abscess.
Managing mastitis
Start treatment as soon as you notice a lump, sore spot or red area on your breast. Early action will help you to feel better faster.
Keep breastfeeding
It's important to keep removing milk from the sore breast to prevent it from becoming overfull and to maintain your supply.
Continue to breastfeed your baby as often as they need.
Make sure they're well positioned and attached.
Start each feed on alternate breasts.
If your baby isn't breastfeeding well, you may need to express.
Your breastmilk is safe for your baby to drink even if you have mastitis. Some babies refuse the breast for a short time because the milk may taste saltier. If this happens, there are ways to encourage feeding.
There are a number of ways you might choose to hold your baby to feed. If your breast is sore and your usual position is uncomfortable, try some other positions.
Help the milk to flow
Sometimes milk flows more slowly from a sore breast, making your baby fussy. Try some of these tips to help the let-down reflex work and your milk to flow more easily:
Loosen your bra or take it off.
Choose a comfortable position that helps you to relax.
Breathe deeply and evenly.
Listen to soothing music.
Hold your baby skin-to-skin.
Gently stroke your breast towards the nipple before a feed.
Warm your breast just before a feed. A warmed gel pack or cloth are easy options. Don't use warmth at other times as it can worsen inflammation.
If your breast still feels full after a feed, express until it feels more comfortable.
Treat inflammation
Cold relieves pain and swelling. Use covered cool packs on the affected breast between feeds. You can make your own cool packs by soaking and freezing breast pads or nappies.
Common anti-inflammatory or pain relief medications can help. Ask your doctor or pharmacist for advice.
Rest and recover
Rest as much as possible, drink plenty of water and eat well. Stay in bed if you can or put your feet up for most of the day. Keep your baby and everything you need close by including supplies for changing nappies and your own food and drinks. If you have other children, it may be easier to rest in your living area.
When to seek medical help
See a doctor if you don't start to feel better (or get worse) within 12 to 24 hours, or sooner if you feel very unwell. You may need medication for pain and inflammation. If you’re prescribed antibiotics, it’s safe to continue to breastfeed - just make sure to finish the course. Some mums may get a thrush infection after taking antibiotics. If you’ve had thrush before, discuss this with your doctor.
If mastitis isn't treated promptly, a breast abscess may form, though this isn’t common.
Preventing mastitis
- Make sure your baby is positioned and attached well to help them remove milk easily.
- Let your baby feed for as long and as often as they want to. If your nipples feel sore you can take your baby off the breast as soon as they stop sucking and swallowing or fall to sleep.
- Treat sore or damaged nipples promptly.
- Start each feed on alternate breasts to ensure milk is removed from both breasts often.
- If your breasts become uncomfortably full, wake your baby for a feed.
- If your baby isn't feeding well at the breast, express to replace missed feeds.
- Rest, drink to your thirst, and eat nutritious foods—being “run down” can increase your risk.
- If you're weaning, do it gradually over several weeks.
- Avoid expressing extra milk if your baby is feeding well.
- Don’t give your baby other fluids except your breastmilk, unless medically advised.
© Australian Breastfeeding Association October 2025
- Deng, Y., Huang, Y., Ning, P., Ma, S. G., He, P. Y., & Wang, Y. (2021). Maternal risk factors for lactation mastitis: A meta-analysis. Western Journal of Nursing Research, 43(7), 698–708. https://doi.org/10.1177/0193945920967674
- Lai, B. Y., Yu, B. W., Chu, A. J., Liang, S. B., Jia, L. Y., Liu, J. P., Fan, Y. Y., & Pei, X. H. (2021). Risk factors for lactation mastitis in China: A systematic review and meta-analysis. PloS One, 16(5), e0251182. https://doi.org/10.1371/journal.pone.0251182
- Mitchell, K. B., Johnson, H. M., Rodríguez, J. M., Eglash, A., Scherzinger, C., Zakarija-Grkovic, I., Cash, K. W., Berens, P., Miller, B., & Academy of Breastfeeding Medicine (2022). Academy of Breastfeeding Medicine clinical protocol #36: The mastitis spectrum, revised 2022. Breastfeeding Medicine, 17(5), 360–376. https://doi.org/10.1089/bfm.2022.29207.kbm
- Shalev Ram, H., Ram, S., Wiser, I., Tchernin, N., Chodick, G., Cohen, Y., & Rofe, G. (2022). Associations between breast implants and postpartum lactational mastitis in breastfeeding women: Retrospective study. British Journal of Obstetrics and Gynaecology, 129(2), 267–272. https://doi.org/10.1111/1471-0528.16902
- Wilson, E., Wood, S. L., & Benova, L. (2020). Incidence of and risk factors for lactational mastitis: A systematic review. Journal of Human Lactation, 36(4), 673–686. https://doi.org/10.1177/0890334420907898
Read more about breast and nipple care
Evidence-led info and practical tips from our Breastfeeding Information Series
Breastfeeding: Breast and nipple care