You can breastfeed after an epidural. Here’s how to make it work for you and your baby.
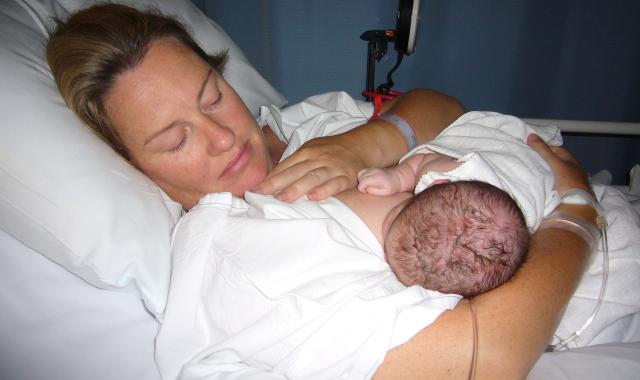
If you’re wondering whether having an epidural will affect your breastfeeding journey, you’re asking an important question. The way you give birth and the pain relief you have can both influence your early breastfeeding experiences.
However, with right information and support, any effects are usually short-lived. Here’s what to expect, what you can do and how to get support if you need it.
What is an epidural or spinal anaesthetic?
An epidural or spinal is a way to manage pain during labour or caesarean birth. It involves a small tube or needle placed in your back to deliver pain relief. The medication is usually a mix of local anaesthetic (to numb nerves) and a small amount of opioid (for extra pain control).
Most medications given during labour can pass from you to your baby, including those used in epidurals. But the doses used in epidurals are much smaller than those given by injection or IV, so less medication reaches your baby.
How might an epidural or spinal affect breastfeeding and what helps?
If you receive an epidural or spinal, you will still be able to breastfeed. However, some types of pain relief and the way birth unfolds can shape the early days of breastfeeding and you may need additional help and support. A few things to be aware of:
- Higher doses of fentanyl (the most common opioid in epidurals) may affect breastfeeding, but lower doses usually don’t.
- Some babies may be sleepier at first and take longer to be interested in attaching to the breast.1 Hold your baby skin-to-skin as much as possible. In time your baby will become more alert and start moving around and showing feeding cues.
- An epidural may affect your natural oxytocin release2 (oxytocin triggers the let-down reflex and helps with bonding). You can boost your oxytocin levels by having lots of skin-to-skin contact with your baby. Other things that help are gentle touch or massage (like stroking your arm or a gentle back rub from your support person), and creating a calm, private space (dimming the lights, limiting noise and visitors).
- While the medications in your epidural gradually wear off, you might need support to get yourself and your baby into a comfortable position to breastfeed.
- For some mums, milk takes a little longer to increase in amount and change from colostrum to mature breastmilk (sometimes called your milk ‘coming in’).1 There’s no need to do anything special, just keep feeding your baby as often as possible and it will happen.
Supporting breastfeeding: your pain relief choices and practical tips
While there are some things to be aware of, it’s important to remember that having an epidural is a valid choice for managing pain during labour. With the right support, most mums and babies do well, and you shouldn’t let worries about breastfeeding stop you from choosing the pain relief you need.
What to do
After the birth, aim for skin-to-skin contact for at least 90 minutes if possible. This helps your baby get to know your feel and smell and helps them find your breast more easily. From then on, keep your baby close, offer the breast as often as you can, hand express if needed, and ask for support. Most early effects are short-lived when you have the right help.
Getting the support you need
- Speak to your antenatal midwife or educator about your options for pain relief in labour and getting support to minimise breastfeeding barriers.
- Learn as much as you can about breastfeeding before birth. Attend a Breastfeeding Education Class if there’s one available locally or a live-streamed interactive Breastfeeding Preparation Session webinar.
- If you have trouble, reach out for support. An ABA breastfeeding counsellor can talk you through helping your baby attach and feel well and how to tell if they’re getting enough milk.
© Australian Breastfeeding Association February 2026
- Andrew, M. S., Selvaratnam, R. J., Davies-Tuck, M., Howland, K., & Davey, M.-A. (2022). The association between intrapartum interventions and immediate and ongoing breastfeeding outcomes: An Australian retrospective population-based cohort study. International Breastfeeding Journal, 17(1), Article 48. https://doi.org/10.1186/s13006-022-00492-7
- Uvnäs Moberg et al. (2020): Maternal plasma levels of oxytocin during breastfeeding—A systematic review. PLOS ONE 15(8):e0235806. https://doi.org/10.1371/journal.pone.0235806
Read more about epidurals and caesarean births
Evidence-led info and practical tips from our Special Situation Information Series
Breastfeeding: Caesarean births and epidurals