With information and support, you can breastfeed your baby.

Breastfeeding is important for babies. You probably already know this and you may be worried about how to provide breastmilk now you know your baby has a cleft of the lip and/or palate.
The most important thing to know is that even if your baby can’t breastfeed at first, you can still feed your baby your own breastmilk.
You may be able to learn how to breastfeed your baby from birth, or over time, using assisted techniques such as using different ways to hold your baby, breast compressions, a supply line, a nipple shield or a combination of these.
When you are in hospital with your baby, there will usually be staff and equipment available to help you express (or pump) milk for your baby. However, you may need to look for a professional who has experience with breastfeeding babies with clefts.
If you are feeling stressed or upset, it may seem easier not to breastfeed or express milk to feed your baby. Family or friends may also think that it will be easier for you to feed your baby formula, but the choice is up to you.
The importance of breastmilk and breastfeeding for babies with clefts
Formula-fed babies have more infections. Babies with a cleft palate can have ear infections more often than other babies, as the Eustachian tubes (that go from the back of the nose to the ear) can fill with milk when they swallow. 1 Breastmilk has important immune-protective factors that are not in formula. Protection from infection is also very important for babies who need surgery.
Breastfeeding helps your baby’s face and jaw to develop well. When baby sucks at the breast, it exercises their facial muscles.2
Breastfeeding helps bonding. Breastfeeding gives your baby lots of cuddling and skin contact and helps you get to know each other. Babies with a cleft often need extra care. Many mothers find breastfeeding their baby helps build a loving and trusting relationship.
Breastfeeding has post-surgery benefits. Breastmilk contains lysozyme and epithelial growth factors that help to stop wounds getting infected.3 Many babies are allowed to breastfeed straight after surgery.4 Breastfeeding is comforting for your baby and your soft nipple will not hurt or damage their mouth.
There are many other reasons why breastmilk and breastfeeding are important for you and your baby.
Breastfeeding your baby with a cleft
Breastfeeding with a cleft of the lip
Babies with a cleft of the lip only can usually breastfeed as a newborn. You can use your breast or fingers to block the cleft to help your baby to get proper suction.
Breastfeeding with a cleft of the soft palate
A cleft of the soft palate is often hard to see. It may only be found after a few hours or days when your baby seems unable to breastfeed. The baby may make a clicking sound while breastfeeding or slip off the breast. The cleft will cause a break in the seal, which is needed for a ‘good’ breastfeeding ‘technique’.
Breastfeeding with a cleft of hard and soft palate
The hard and soft palate may be cleft unilaterally (one side) or bilaterally (both sides). Breastfeeding is most difficult for babies with a cleft of the hard palate. Learning to breastfeed may take a long time and will most likely need some assisted techniques and/or lactation aids. Your baby will use a lot of energy breastfeeding. They may need more kilojoules so that they keep growing well. These extra kilojoules could be from expressed breastmilk given by a special cup or feeder.
All babies want to suckle frequently after birth. Your baby does not know they have a cleft and your breast is the perfect soft shape for them to suckle. In time your baby will learn to fill the cleft with your breast as they become better at feeding and you will soon learn how to help them to breastfeed.
Even if your baby is getting most of their milk from a cup or feeding bottle, this practice will exercise baby's muscles and help them get ready for breastfeeding once the cleft is repaired.

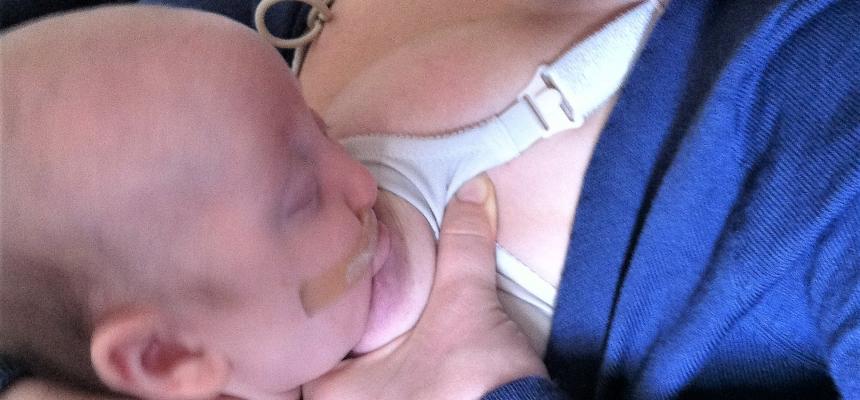
Tips for breastfeeding
Any time your baby spends at the breast is helpful.
Breast compressions help to increase the flow of milk to your baby.
Comfort sucking and feeding to sleep are important to your baby for both food and learning.
To help form a seal and keep suction, hold your breast in your baby's mouth by pressing with the index and middle finger on the breast, well back from the nipple, making the breast protrude as if full of milk.
Keep your baby's head close to the breast throughout the feeding.
Take each day as it comes. Try not to feel guilty if, at times, breastfeeding is hard work and you feel annoyed or sad. With time it can get easier.
Be flexible and persistent so you can adapt to your baby's changing needs. Knowing how fast babies grow up may help you cope better.
Reward yourself for not giving up and for all your hard work. Allow yourself a treat now and then. You’ve earned it!
Tips for expressing
Most mothers can make enough milk to meet their baby's needs. The more milk you express, the more you will make. Your baby's milk needs don’t increase much from 1 to 6 months of age.5 This means you won’t need to keep increasing the amount of expressed milk as your baby grows bigger. However, you may find your baby needs extra milk after surgery, as they recover.
Regular expressing is important. You need to keep your supply going by expressing your milk as often as your baby would normally feed.
Expressing during the night is important for your milk supply during the early months.
Consider hiring an electric breast pump, possibly one with a double kit so you can pump both breasts at once. ABA members receive a discount on breast pump hire costs.
Encourage your let-down reflex. It's important for your baby to get as much breastmilk as you can manage to express, even if they are also having some formula. You can increase your milk supply by expressing milk from your breasts more often.
Coping with wind, colic and regurgitation
Many babies with clefts have wind or colic problems because they swallow more air than other babies. This can happen whether they are breastfed, breastmilk-fed or fed with formula.
These ideas may help:
Feed in an upright position.
Burp baby often during feeding.
Carry baby upright in a sling.
Massage your baby.
Regurgitation or vomiting of milk (or solid foods in later months) through the nose is also common. It will stop once the palate is repaired. Breastmilk will not hurt the lining of your baby's nose.
Your child health nurse, lactation consultant and your ABA counsellor can provide you with information and support as you breastfeed and/or express. They may be able to put you in contact with another mother of a baby who has had a cleft or refer you to the CleftPALS organisation.
However you decide to feed your baby, there is support available to help you.
Bottles, teats and other feeding equipment
There are several bottles and teats designed for babies with cleft palates. The most common method of feeding is to use a 250 mL polythene squeeze bottle. The teat is placed on your baby's tongue and the flow of milk increased by gently squeezing the bottle. You can pace the squeezes to the rate your baby can drink the milk.
However, it is important that baby doesn’t get the milk too quickly and easily as they need to learn the suck-swallow-breathe pattern. Trying to drink too fast can make your baby gag, cough and splutter or regurgitate (vomit). 'Working' for the milk will also help your baby to develop their facial muscles and a strong sucking response.
Medela Special Needs (previously called Haberman) Feeder. This is a bottle specially designed for any baby with a poor suck.
Dr Browns Bottle and teat and valve
Pigeon squeezy bottle
The Softplas squeeze bottle manufactured by Douglas Bean (Australia) Pty Ltd
CleftPALS Qld Inc squeeze bottle
Chu Chu
Pur Simplicity teats, fast flow for 6-18 months
Pigeon cleft palate teat and valve
Using a combination of Chu Chu teat with Pigeon valve
Nuk rubber, fast flow for thick foods, x-cut teats
Nuk feeding spout
As with any baby who is bottle-fed, you may need to try different teats or spouts to find the one that works best for you and your baby.
(used in conjunction with breastfeeding or on its own)
Syringe Feeding is often used when the majority of the feeds are done at the breast.
Spoon Feeding can often be slow at first, but with experience it can speed up.
Nipple Shields can be of use when the baby is struggling to attach or has got used to a bottle teat. They can be used in combination with breast compressions.
Cups - the Softplas squeeze bottle manufactured by Douglas Bean (Australia) Pty Ltd comes with a number of feeding spouts and scoops that can be used for cup-feeding.
The Medela Softcup Feeder.
Hear from other mums
Kathryn had a cleft of the soft palate and slightly into the hard palate. I was unable to breastfeed her as she could not make enough suction to milk the breast. I expressed for 12 months. Kathryn was exclusively breastmilk-fed for 7 months, then continued to have breastmilk along with other food until 12 months of age. She was a healthy baby and is a very active, healthy toddler. I found expressing the milk was the easy part, but feeding it to her was hard.
We started with a squeezy bottle and a normal teat. We went through over 15 different types of teats but she still couldn't feed properly. We eventually used a Haberman Feeder. It cut feeding times down from 90 minutes to 20–30 minutes. When I wanted to increase my supply I would express more often and I would start to see an increase by day 4. Expressing for my daughter was very rewarding. Sometimes I felt like it was the one positive thing I could do for her. It was particularly good for both of us after her surgery. She had a very fast recovery with no infections and did not need much pain relief.
Rebecca had a cleft of the soft and hard palate diagnosed on day three. I was unaware of assisted breastfeeding techniques and as she had a collapsed lung at birth she struggled to take fifty percent of her bottle, so for the first three months we also used a nasal gastric tube to compliment her feeds until we could see a cleft specialist at three months of age. Weaning her off the nasal gastric tube was challenging and ended up requiring short term medication to stimulate her appetite.
At first we used a Haberman feeder, then we trialled the squeeze bottle with the Chu Chu teat and pigeon valve. During this time I expressed four to six times a day with ten minute pumping sessions, the frequency of sessions reflected the number of feeds a normal breastfed baby may have. I was able to keep a strong supply going with the aid of a toddler who was still breastfeeding and some medication.
At nine months she had her surgery, which was successful. Determined not to give her another bottle and to get her on the breast, I spoon fed her liquid and purees the first four weeks, we then used a supply line and nipple shield for the next five weeks until one evening she proved that could breastfeed unassisted. All up I expressed for my daughter for eleven months. At thirteen months of age the breastfeeding is still going well and it is such a joy, and such a delight and time saver no longer having to pump.
Further resources and support
CleftPALS (Cleft Palate and Lip Society)
CleftPALS is a support organisation in each state. It consists of professionals and parents involved in the treatment of the cleft condition. Volunteers from CleftPALS offer support and guidance to new families all over Australia.
(NSW) Cleftpals NSW www.cleftpalsnsw.org.au
(QLD) CleftPals Queensland www.cleftpalsqld.org.au
(VIC) CleftPals Victoria https://www.cleftpalsvic.com/
(WA) CleftPals WA https://www.cleftpalswa.org.au/
The Royal Children’s Hospital Melbourne Cleft lip and palate – infant feeding
Cleft lip and palate services at The Children's Hospital at Westmead
Cleft Connect Australia https://cleftconnect.org.au/
© Australian Breastfeeding Association April 2022
1. Aniansson, G., Svensson H., Becker, M., Ingvarsson, L. 2002, Otitis media and feeding with breast milk of children with cleft palate. Scand J Plast Reconstr Surg Hand Surg 36(1):9–15.
2. Gomes, C., Trezza, E., Murade, E., Padovani, C. 2006, Surface electromyography of facial muscles during natural and artificial feeding of infants. J Pediatr (Rio J) 82(2):103–109.
Raymond, J., Bacon, W. 2006, Influence of feeding method on maxillofacial development. Orthod Fr 77(1):101–103.
3. Shah, P., Aliwalas, L, Shah, V. 2007, Breastfeeding or breastmilk to alleviate procedural pain in neonates: a systematic review. Breastfeeding Med 2(2):74–82.
4. Darzi, M., Chowdri, M., Bhat, A. 1996, Breast feeding or spoon feeding after cleft lip repair: a prospective randomised study. Br J Plast Surg 49:24–26
Cohen, M., Marschall, M., Schafer, M. 1992, Immediate unrestricted feeding of infants following cleft lip and palate repairs. J Craniofac Surg 3(1):30–32.
5. Kent, J.C., Leon, M.R., Cregan, M.D., Ramsay, D.T., Doherty, D.A., Hartmann, P.E. 2006, Volume and frequency of breastfeeding and fat content of breastmilk throughout the day. Pediatrics 117(3):e387–e395.
Read more about breastfeeding your baby
ABA booklets - for evidence-led info and practical tips
Breastfeeding: your baby with cleft of lip and/ or palate